By understanding the spectrum of injuries, particularly upper extremity fractures, that occur with intimate partner violence (IPV), radiologists can be first-line advocates for women and men who are enduring abuse, even when the abuse goes unreported by the patient.
“I think the most difficult aspect of treating IPV is that recognizing it is hard,” said David Sing, MD, a third-year orthopedic resident at Boston Medical Center. “There aren’t guidelines or a standardized reference; there is little to no education on IPV during medical school.”
As part of a scientific session at RSNA 2020, Dr. Sing presented research comparing patient characteristics and radiographic features associated with isolated ulnar fractures in IPV-related and non-IPV-related cases. The multicenter study was performed at the Trauma Imaging Research and Innovation Center (TIRIC), Brigham and Women’s Hospital, Boston. “We looked at data from six different hospitals, including females aged 18 to 50 who sustained isolated ulnar shaft fractures,” said Dr. Sing.
The researchers examined patient demographics, as well as history and risk factors. They also explored whether there was a report of screening for IPV at the initial visit, the number of documented emergency visits in the past, and what the patient—or any witnesses—reported as the mechanism of injury. They found that approximately 26% of cases in patients with isolated ulnar fractures were attributable to IPV.
“In my first year as a resident, I saw a 34-year-old woman who said that she fell,” said Dr. Sing. “I thought this was a non-displaced, isolated ulnar shaft fracture. The radiology reports agreed. I know now that we could have done a better job in taking a more thorough history, or at least asking if she felt safe at home.”
“We need to move beyond patients’ self-reporting and find ways to identify victims sooner,” said Richard Thomas, MD, a former fellow at the Brigham and Women’s Hospital and an attending radiologist at Lahey Hospital and Medical Center in Cambridge, MA. “This is particularly important now during the pandemic, which has exacerbated the incidence and severity of physical abuse.”
Dr. Thomas presented research performed at TIRIC that included both men and women who were referred to the intimate partner violence support program at Brigham and Women’s Hospital with a history of physical IPV between January 2013 and June 2018. The team found that upper extremity injuries in victims of IPV most commonly occurred in the hand and finger region, and that up to one fifth of patients had recurrent upper extremity injuries.
“Finger fractures do not often occur with a fall, although ‘fall’ was the most commonly reported mechanism of injury among our patients who did not disclose IPV. Therefore, finger fracture with an unclear history of fall should raise the suspicion of IPV,” Dr. Thomas said.
Drs. Thomas and Sing presented their findings as part of the RSNA 2020 science session, “Emergency Radiology Trauma: Head, Spine, and Extremities,” featuring a keynote by Bharti Khurana, MD on the role of the radiologist in detecting IPV. Dr. Khurana is the founding director of TIRIC and the principal investigator for both studies.
Dr. Thomas’s team found that only 17% of the patients in their cohort had disclosed a history of IPV at the time of injury, and that IPV screening was documented in only 25% of cases. “Furthermore, 35% of these patients never had any documentation of IPV in their health record even though all patients subsequently reported IPV to our institution’s violence prevention support program,” Dr. Thomas said. “This underscores the key role that radiologists can play by identifying these patients based on stigmata of abuse visible on radiological studies.”
“We believe that by being aware of these patterns, and by reviewing prior and concomitant imaging studies, radiologists can help raise the possibility of intimate partner violence and facilitate early intervention to break the cycle of abuse,” said Dr. Khurana.
For More Information
View the RSNA 2020 session Recognizing Intimate Partner Violence: Defensive Ulnar Fractures and Upper Extremity Injuries in the Victims of Intimate Partner Violence — SSER02 at RSNA2020.RSNA.org.
Has your institution seen an increase in intimate partner violence cases since the pandemic?
— RSNA (@RSNA) November 30, 2020
To learn more about this topic, check out SSER02-02/04: Recognizing Intimate Partner Violence. #RSNA20
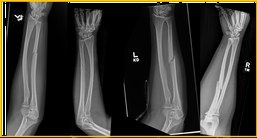
Isolated ulnar fractures, as demonstrated above, are uncommon injuries that are red flags for intimate partner violence.
Anteroposterior (figure A) and lateral (figure B) radiographs of the left hand in a 30-year-old female with reported history of assault by intimate partner show a minimally displaced fracture of the shaft of the fifth metacarpal, with overlying soft tissue swelling (arrows).
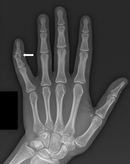
Anteroposterior radiograph of the left hand in a 36-year-old female with reported history of assault by intimate partner shows a mildly displaced fracture of the middle phalanx of fifth digit, with overlying soft tissue swelling (arrow).






